INTRODUCTION
Thyrotoxicosis is a syndrome caused by excessive levels of thyroid hormones in the blood and their toxic impact on various organs and tissues. The prevalence of thyrotoxicosis in Russia in 2001 was 18.4 cases per 100,000 [1]. According to the American Thyroid Association (ATA), the prevalence of thyrotoxicosis in the USA in 2011 was 1.2–1.6%, 0.5–0.6% for overt forms and 0.7–1.0% for subclinical forms [2]. The most common cause leading to thyrotoxicosis in regions with normal iodine intake is Graves’ disease. The most common cause in iodine-deficient areas is autonomously functioning thyroid nodules [3]. Other causes of thyrotoxicosis are ectopic thyroid tissue; thyrotoxic phase of destructive thyroiditis; medication, most often amiodarone; and overdose of thyroid hormones, for example, in the treatment of hypothyroidism. Drug-induced thyrotoxicosis can also occur in the case of uncontrolled intake of hormones by patients suffering from a mental illness, including eating disorders [4].
Eating disorders (EDs) are widespread in the population. According to our estimates, the prevalence of anorexia nervosa ranges from 0.3 to 1% and the prevalence of bulimia nervosa ranges from 0.9 to 1.5% [5]. The problem cannot be underestimated, since the mortality rate among this category of patients is the highest relative to other psychiatric disorders: according to statistics, about 23 patients die daily from EDs [6] and almost 20% of patients commit suicide [7]. Studies have shown that people with eating disorders have a characteristic personality type: emotional lability, a tendency to maladaptive behaviors, a constant feeling of internal tension and discomfort, low self-esteem, and a desire for hyper-control [8, 9]. Often, eating disorders are comorbid with other psychiatric diseases, including schizophrenia spectrum disorders, as well as mood disorders [10].
The desire to lose weight by patients with EDs is often associated with maladaptive behavioral strategies, including the abuse of various drugs [11, 12]. These include diuretics and laxatives, as well as hypoglycemic and hormonal drugs. Often, these are thyroid hormone drugs that can accelerate the matabolism, and, consequently, lead to weight loss. Unfortunately, the abuse of these drugs also leads to cardiovascular, metabolic, and endocrine disorders [13]. The issue is complicated by the wide availability of these drugs, which are often classified as over-the-counter medications. At the same time, proving the fact of drug abuse may not be the easiest of tasks and may require a comprehensive clinical examination, including examining a detailed medical history, performing a wide range of investigative steps, and soliciting consultations from specialists in related fields.
The presented clinical case describes drug-induced thyrotoxicosis resulting from the self-administration of large doses of levothyroxine by a patient with anorexia nervosa in an effort to reduce body weight.
Drawing one’s attention to the problem of a transnosological search taking possible mental disorders in patients with medical symptoms into account, in our opinion, will optimize the diagnostic process, accelerate it, and improve its accuracy.
PATIENT INFORMATION
A 20-year-old female patient came to an endocrinologist at the Central Clinical Hospital of Civil Aviation (CCH CA) in July 2021 to check for thyrotoxicosis before a planned thyroidectomy for diffuse toxic goiter. She complained of constant palpitations (heart rate of up to 150 bpm), periodic episodes of tachycardia of up to 200 bpm lasting up to 10 minutes and inadequately relieved by β-blockers (propranolol up to 40–50 mg), sweating, tremor, and lack of menstruations. The patient had been experiencing these symptoms since 2020.
At examination: increased heart sounds; heart rate of 180 bpm, blood pressure 130/70 mm Hg, height 160 cm, weight 49 kg, and body mass index (BMI) = 19.1 kg/m2. The thyroid gland is not palpable; von Graefe’s, Moebius, Chvostek’s, and Trousseau signs are negative. The patient has trunk and limb tremor while standing.
Due to tachycardia of 180 bpm not relieved by propranolol 40–50 mg, general tremor and increasing weakness at the time of examination in the Admission Department, the patient was hospitalized in the Intensive Care Unit (ICU) in serious condition, followed by a transfer to the Endocrinology Department with a diagnosis of thyrotoxicosis.
MEDICAL HISTORY
According to the medical history, in 2017 the patient was treated in a psychiatric hospital for anorexia nervosa after a weight loss of 30 kg in a year (from 70 to 40 kg); the development of amenorrhea. After treatment in a psychiatric hospital (there is no information on the patient taking psychopharmacological drugs after discharge), the patient gradually gained weight up to 49 kg while her menstrual cycle did not resume.
Family medical history is unremarkable; the patient denies smoking, alcohol or substance abuse, injuries, or allergic reactions. There were no pregnancies. The patient is a student of the pharmacological faculty of a medical institute. The timeline of the patient seeking medical attention is presented in Figure 1.
Figure 1. Timeline of the patient seeking medical attention.
Results of previous clinical examinations
The first thyroid function tests were performed in July 2020. They revealed a decrease in the thyroid-stimulating hormone (TSH) to 0.005 μIU/mL (normal range 0.4– 4.0 μIU/mL) and an increase in free T3 (25.5 pmol/L, normal range 3.1–6.8 pmol/L) and free T4 (40.5 pmol/L, normal range 10.8–22.0 pmol/L). The level of antibodies to thyroglobulin (Ab-TG), Ab to thyroid peroxidase (Ab-TPO), and Ab to TSH receptors (TSHr) were within the reference range.
Thyroid gland (TG) ultrasound from July 2020 showed ECHO-signs of moderate diffuse changes in the thyroid gland, an emerging node of the right lobe; the total volume of the thyroid gland was 7 cm3.
Scintigraphy of the parathyroid glands and the thyroid gland with Technetril was performed at the same time. The following conclusion was made: “No scintigraphic signs of parathyroid gland adenoma.”
After 2 weeks, during repeated scintigraphy with pertechnetate, no image was obtained on the thyroid gland scintigram. The uptake of the radiopharmaceutical (RP) in the submandibular and cervical lymph nodes was within the normal limits. It was recommended to repeat the study of the thyroid gland with a more thorough preparation of the patient within 3–4 months. The following conclusion was made: “Blocked thyroid gland.”
The patient was consulted by an endocrinologist who, based on investigations, diagnosed Graves’ disease and recommended thiamazole at a dose of 30 mg/day, which the patient reportedly took at the prescribed dose until March 2021.
Bone densitometry was performed in July 2020. It revealed low bone mineral density for the chronological age (Z-score >-2.0 SD).
A complete gynecological examination revealed uterine hypoplasia and multifollicular ovaries. The androgenic profile included an increased level of sex-hormone-binding globulin (SHBG) up to 264 nmol/L (the normal range is 32.4–128 nmol/L). The following diagnosis was made: “Secondary normogonadotropic amenorrhea associated with thyrotoxicosis. Osteopenia without pathological fractures. Hypophosphatemia. Neutropenia. Latent iron deficiency.”
In March 2021, during antithyroid therapy with thiamazole, a blood count revealed neutropenia with a decrease in absolute neutrophils to 1.36×109/L (the normal range is 1.5–6.3×109/L). The antithyroid agent was discontinued; prednisolone 15 mg/day and metoprolol 50 mg BID were prescribed.
In May 2021, the patient underwent surgical treatment in the Ear, Nose and Throat (ENT) Department: posterior inferior conchotomy, septoplasty, and submucosal vasotomy of the inferior turbinates. Before hospitalization for surgical treatment, all laboratory parameters were within the reference values, the ECG showed sinus arrhythmia, and there was a normal heart rate (63–85 bpm). The surgery and postoperative period proceeded without complications. The patient was discharged from the hospital in satisfactory condition. Shortly after his discharge, palpitations, sweating, and tremors resumed.
In June 2021, a second thyroid function test was carried out: TSH 0.0083 μIU/mL, free T4 63.3 pmol/L, free T3 16.3 pmol/L, Ab to TSHr 19.05 IU/L (the normal range is less than 1.75 IU/L).
A decrease in serum iron to 4 µmol/L (the normal range is 7–25 µmol/L) was also revealed. It is known that, because of the indicated changes in the laboratory parameters, the patient was consulted by an endocrinologist for an expert assessment at the Federal Center for Endocrinology (FCE); the primary diagnosis of Graves’ disease was not changed. The following treatment recommendations were received: propranolol 40 mg at a heart rate of >90 bpm, iron polyisomaltose 50 mg/mL, metoprolol 50 mg 2 BID, lifelong discontinuation of antithyroid agents, and consultation with an endocrinologist-surgeon. Total thyroidectomy had been suggested as a treatment. The patient noted that the recommended therapy was not effective in relation to palpitations: propranolol at a dose of 40–50 mg reduced the heart rate for no more than 10 minutes.
DIAGNOSTICS AND THERAPY
Specialists at the Central Clinical Hospital of Civil Aviation conducted a repeated ultrasound examination of the thyroid gland, as well as ultrasound of the zones of possible ectopia of the thyroid tissue, repeated scintigraphy, complete blood count and blood chemistry tests, study of blood electrolytes and thyroid hormone profile (TSH, T3, free T4, Ab-TG, Ab-TPO, Ab to TSHr) for additional examination in order to verify the cause of thyrotoxicosis.
The following therapy was prescribed: propylthiouracil 300 mg/day, 100 mg/day from day 5, discontinuation from day 9; dexamethasone (16- to 14- to 12- to 8- to 4-mg IV), prednisolone 10 mg/day, then 7.5 mg/day; and metoprolol 50 mg/day, omeprazole 40 mg/day. Specialists at the ICU also conducted infusion therapy in a volume of up to 2 liters (0.9% sodium chloride solution, 5% glucose solution, Haemodez).
Based on the results of thyroid and whole-body scintigraphy with pertechnetate and Technetril, the following conclusion was made: “The thyroid gland is not visualized and whole-body scintigraphy showed no signs of ectopic functioning thyroid tissue” (Figure 2). The absence of Tc-99m-Technetrile in the thyroid gland may indicate a pronounced disorder of the functional state of thyrocytes (destruction?), while the absence of thyroid gland visualization during the study with Tc-99m-Pertechnetate may indicate a blocked thyroid gland.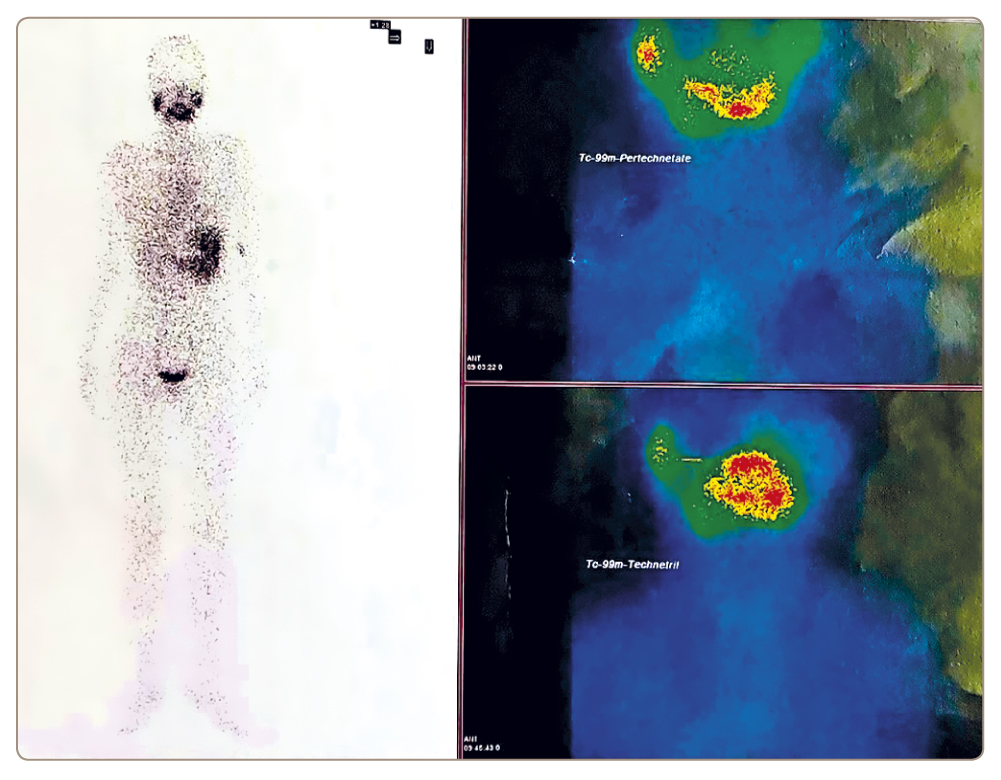 Figure 2. Scintigram with pertechnetate and Technetril.
Figure 2. Scintigram with pertechnetate and Technetril.
Ultrasound of the thyroid gland provided the following data: The total volume is 5.7 cm3. The parenchyma echogenicity is moderate. The echostructure is slightly diffusely heterogeneous. Areas of reduced echogenicity without clear contours (areas of lymphoid infiltration?): single 3 mm on the left, 3–6 mm on the right; vascularization of the parenchyma is not increased. Lymph nodes are not changed. Areas of thyroid ectopia were not reliably identified during the study of the anterior and lateral parts of the neck.
Hormonal status of the thyroid gland at the time of admission to the hospital: free T4 57.6 pmol/L, TSH 0.05 μIU/mL.
Due to the severe condition of the patient because of thyrotoxicosis, therapy with the antithyroid agent propylthiouracil with blood test monitoring, as well as glucocorticoids (dexamethasone IV, then oral prednisolone), β-blockers, was again initiated.
After 10 days of hospitalization, free T4 decreased to 13.3 pmol/L, free T3 remained within the normal range, and TSH was 0.05 μIU/mL. The repeated blood test for antibodies to TSH receptors: 0.8 IU/L (the normal range is 0–1.75 IU/L), and the Ab-TPO level was within the normal range. Complete blood count showed no signs of neutropenia during therapy with antithyroid agents. Electrolytes and serum iron were within the normal range. Heart rate was within 70–76 bpm.
ANALYSIS OF DIAGNOSTIC AND THERAPY RESULTS
Given the results of our investigations at the time of hospitalization and the patient’s medical history, we excluded the previously established diagnosis of diffuse toxic goiter (Graves’ disease), since not a single diagnostic sign corresponded to the course of the said disease: there was no diffuse increase in thyroid volume according to ultrasound results; no increased blood flow to the thyroid gland, increased uptake of radiopharmaceuticals by the thyroid tissue according to scintigraphy; or any antibodies to TSH receptors. There was also no ectopic tissue of the thyroid gland.
Differential diagnosis was carried out with destructive diseases of the thyroid gland, which, like Graves’ disease, are characterized by a decrease in the uptake of radiopharmaceuticals during scintigraphy. However, the long history of the disease in the patient contradicted this assumption: in most cases, destructive thyroiditis does resolve itself spontaneously, with complete recovery [1, 3], which did not happen in this case.
The fact that during the 2-week hospitalization the level of T4 decreased and that the symptoms of thyrotoxicosis quickly decreased speaks not so much to the effectiveness of the therapy as it does to the fact that the patient stopped taking thyroxine in the hospital (the period of elimination of exogenous levothyroxine from the body is 10 days). Given the low body weight of the patient and their history of anorexia nervosa, we made an assumption that the patient was deliberately taking thyroxine to reduce her body weight.
There was a similar case of absolute compensation of the condition in the patient in May 2021 during a hospitalization in the ENT Department, followed by the re-emergence of thyrotoxicosis symptoms after discharge. It can be speculated that back then the state of compensation for thyrotoxicosis was also a result of the inability to take thyroxine in order to reduce body weight in a hospital setting.
We also focused attention to the discrepancy between the result of the test for antibodies to TSHr from June 2021 provided by the patient’s parents and the one provided by the patient herself. The result of the test provided by the parents was negative, while the patient provided results with the presence of antibodies to TSHr. It is also worth considering the fact that the test was performed in a private laboratory, where the result is sent electronically. It is possible that the patient deliberately faked the result of the test to confirm the diagnosis of Graves’ disease. It is known that patients with anorexia nervosa are extremely resourceful in hiding the symptoms of the disease, especially if their intelligence and level of education are high enough [14]. Our patient, being a student of the pharmacological faculty of a medical university, undoubtedly had an idea about thyroxine and its properties, as well as about the typical clinical sings of thyrotoxicosis and its diagnosis.
It is also important to note that during the course of treatment, the attending physician and the authors repeatedly interviewed the patient to clarify the likely fact of drug abuse to maintain low weight. The patient categorically denied taking medications without a doctor’s prescription, which further complicated the search for a diagnostic. The conclusion about drug-induced thyrotoxicosis was made on the basis of the changes in the results of our investigations and the clinical condition of the patient.
The patient was discharged from the Department with a diagnosis of severe iatrogenic thyrotoxicosis.
PATIENT FOLLOW-UP
A month after the patient was discharged from the Endocrinology Department, her mother contacted us; a conversation allowed us to establish that the girl confessed to her parents that she had used thyroxine without a doctor’s prescription in order to lose weight. According to the mother, the patient resumed taking thyroxine due to an increase in body weight by 2 kg and categorically refused to stop the unreasonable use of the drug. The patient refused a consultation with a psychologist or psychiatrist. An explanatory conversation was held with the relatives about the need for psychiatric treatment, but they did not consider it possible to “force” the patient to undergo treatment. However, the relatives intend to contact a specialist in the relevant field privately.
DISCUSSION
The presented case report describes a diagnostic search performed by endocrinologists because of clinical symptoms of thyrotoxicosis in a patient with a history of anorexia nervosa. The peculiarity of this case report was the deliberate concealment of the fact of self-administration of thyroxine by the patient from her doctors, which led to an incorrect medical strategy for this patient at different stages of her medical care. It is known that patients with anorexia nervosa tend to dissimulate the disease, and the resulting medical complications often lead to hospitalization in general hospitals [14].
In a retrospective analysis, conclusions can be drawn regarding the possible acceleration of a correct diagnosis in this patient with an optimal algorithm for diagnostic search and interpretation of investigation results and a comprehensive record of medical history, additional examinations and the effect of drugs.
For example, after the detection of a complete blockade of the thyroid gland on scintigraphy in July 2020, the endocrinologist could have had three diagnostic assumptions:
- The thyroid gland is blocked by iodine taken by the patient;
- The patient has destructive thyroiditis, which is accompanied by a lack of radiopharmaceutical uptake; or
- The thyroid gland is blocked due to the fact that the patient is taking thyroxine; i.e., the thyrotoxicosis is iatrogenic.
Also, in July 2020 when low bone mineral density for the chronological age (Z-score >-2.0 SD) was detected during bone densitometry and a gynecological examination was conducted, normogonadotropic amenorrhea due to thyrotoxicosis was diagnosed without taking the history of anorexia nervosa into account. It is well known that the combination of amenorrhea with osteopenia or osteoporosis is the most common endocrinological manifestations of anorexia nervosa [15].
Performing parathyroid scintigraphy with Technetril seems to be insufficiently justified.
When analyzing the data of previous laboratory tests, it can be concluded that the antithyroid therapy with thiamazole because of thyrotoxicosis carried out from 2020 to 2021 was ineffective. In addition, prescribing a full blocking dose of thiamazole 30 mg in conditions of a completely blocked (according to scintigraphy) thyroid gland was not justified, since there was no target for the drug. Moreover, taking the antithyroid agent at the prescribed dosage until May 2021 led to the development of neutropenia, which could potentially have led to negative consequences for the patient’s health, including death.
We can assume that the presence of antibodies to the TSH receptor, a marker of the autoimmune thyroid disease, misled clinicians into issuing the diagnosis of Graves’ disease. Insufficient critical analysis and rechecking of the information provided by the patient also led to an incorrect diagnosis.
Clinicians should remember that particularly careful monitoring of the behavior of patients is required in the treatment of patients with anorexia nervosa, including covert observation of relatives, medical staff, roommates, and double-checking of the information provided, correlating them with the data of objective examinations [16].
Summarizing the above, it can be concluded that omission of the history of anorexia nervosa at different stages of a patient management path led, in this case, to a number of incorrect diagnostic and therapeutic decisions.
It should be noted that a blood test for thyroglobulin should be performed for a complete differential diagnosis between destructive thyroiditis and iatrogenic thyrotoxicosis.
In our opinion, the case in this report clearly illustrates the complexity of conducting diagnostic and therapeutic work with patients suffering from eating disorders in general medicine.
