Suicidal behavior by children and adolescents is one of the most pressing and painful issues not only in psychiatry and pediatry, but also in society as a whole. It is known that only 5% of suicide attempts in adolescence have psychotic motives, while personality disorders account for up to 20–30%, the remaining causes being found mainly in the so-called “adolescence crises”. The social factors that provoke suicidal behavior in children and adolescents can include difficult situations and chronic conflictual relationships in the family and at school, sexual and physical abuse, experience of domestic violence, parental divorce, death of loved ones, substance abuse, having a family member with a severe mental or physical illness, own illness, and family history of suicide. Acute periods of grief, fallout of violent episodes, bullying, and long-lasting family and social conflicts can lead to the formation of several psychopathological conditions, often complicated by a propensity for self-harming and suicidal behavior. It is known that the vulnerability adolescents present against different, potentially psychogenic factors is much more acute than it is at any other age because of their high emotional vulnerability, the instability of their emotional reactions, weakness of their regulatory mechanisms, and volitional processes that display a deficiency of forecasting and control over one’s own actions. When analyzing the completed suicides among children and adolescents, researchers from different countries have come to conclude that conflict in the family environment is the main trigger in those who commit suicide. Children from single-parent families or children that have difficult relationships with their parents are at the highest point of risk as regards suicide. About 5% of survivors of childhood abuse attempt suicide within 10 years of the experience, and more than 36% of them repeat the suicide attempt within 20 years. At the same time, a parent that attempts suicide can result in an almost 5-fold increase in the likelihood of children committing suicide.
According to the WHO, the worldwide suicide rate averages 10.5 (13.7 for men and 7.5 for women) per 100,000 population, ranging from 5 to 30 per 100,000 population in different countries. About 800,000 people die by suicide each year [1]. In adolescents aged 15–19, suicide becomes the second (for girls) and third (for boys) cause of death, second only to traffic accidents and homicide [2, 3]. It is believed that, for every completed youth suicide, there are 100–200 suicide attempts [4]. By age 18, about 4.1% of adolescents have made at least one attempt at suicide [5]. In the Russian Federation, annually one in 12 teenager makes a suicide attempt, after which the risk of repeated suicide attempts increases by 10–15 times in comparison with the general population [6].
Suicide attempts remain not only the most important risk factor for committing suicide in the future, but they also lead to hospitalizations, injuries, inability to work, and disabilities, putting a heavy financial burden on society.
Therefore, as the WHO stresses, the prevention of suicidal behavior is a global imperative for the whole world [1].
Suicidal behavior is a biopsychosocial problem in which the biological, psychological/psychopathological and social aspects are equally implicated. Prevention, help, and rehabilitation of children and teenagers with suicidal behavior is a multidisciplinary problem.
Thus, it is known that one of the major factors that influence the occurrence and progression of suicidal thoughts and intentions is a depressive syndrome of varying etiologies, from psychogenic to endogenous and exogenous-organic.
Depression in children and adolescents has been found to increase their risk of suicide attempt by 6 times compared to the general population [5]. Approximately 14–25% of children and adolescents have experienced at least one depressive episode by the time they reach adulthood [7]. According to the British Epidemiological Society, 41% of children aged 11 to 15 with depressive disorders have attempted suicide [8].
Nevertheless, the scholarship of the motives of suicidal behavior indicates that a large role is played by micro- and macrosocial factors. The social factors likely to lead to suicidal behavior in children and adolescents can run the gamut of acute situations and chronic conflict relationships in the family and school, sexual and physical violence, being a witness of domestic violence, parental divorce, death of loved ones, substance abuse, having a family member with a severe mental or physical illness, somatic illness, suicide history in the family [9, 10]. Therefore, effective help to an adolescent displaying suicidal behavior is possible only through a multidisciplinary approach, with the participation of the psychiatrist, psychologists, and, in some cases, specialists in social welfare, police, etc.
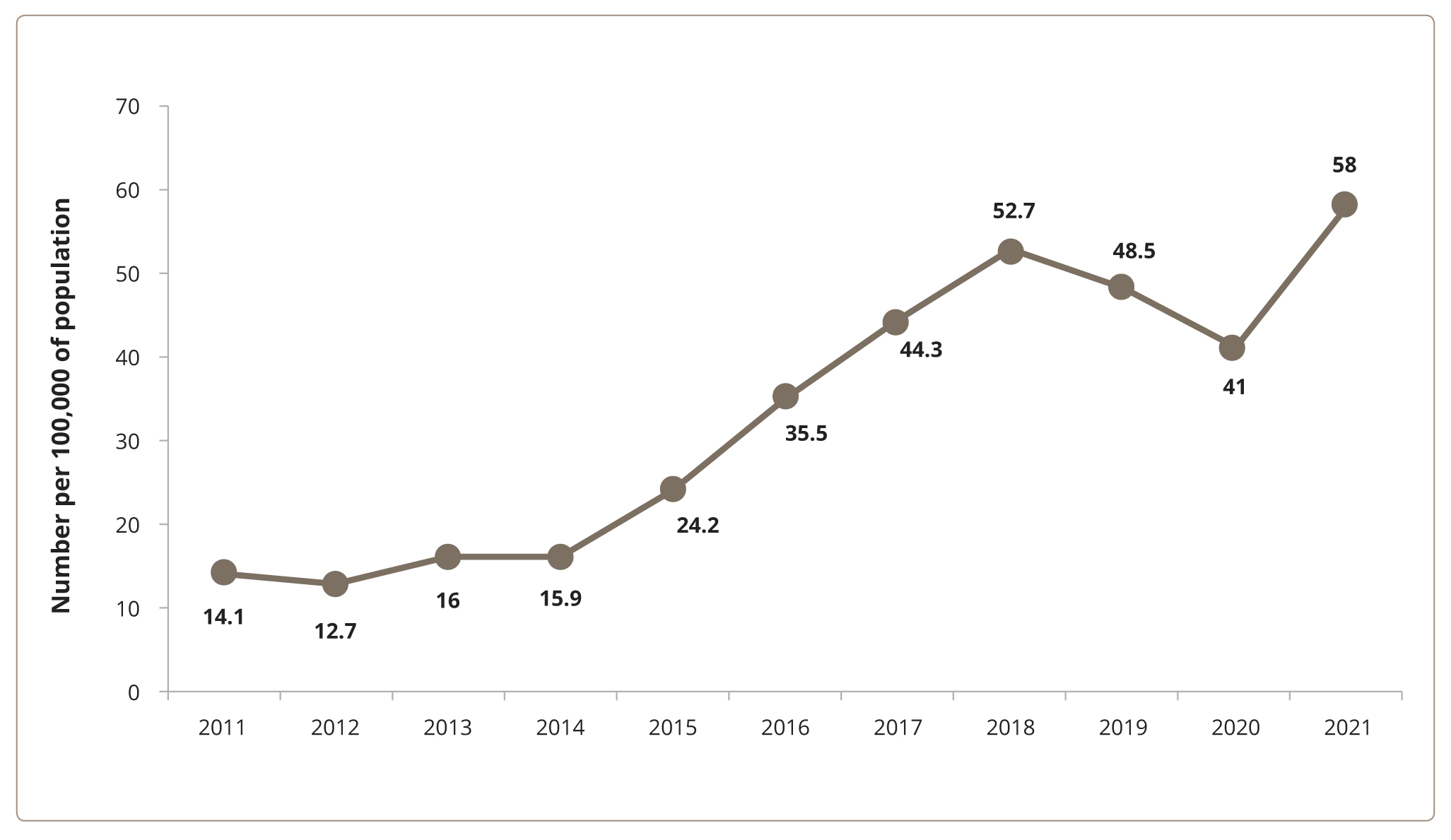
A look at the medical records of the Sukhareva Сenter indicates an increase in hospitalized adolescent patients with suicidal behavior. This reflects the dynamics of suicidal behavior in Moscow as a whole, since the Sukhareva Center is the only ambulance psychiatric hospital in the city (Figure 1).
Figure 1. Number of children and adolescents displaying suicidal behavior per 100,000 of Moscow’s child population.
Of course, these figures are likely an underestimation, since not all children and adolescents with suicidal behavior are seen by a psychiatrist. Indirectly, the scale of the problem can be assessed through the number of corresponding inquiries on the Internet. In 2020, 833 adolescents with suicidal behavior were hospitalized at the Sukhareva Center while the number of search queries in Moscow on the Yandex platform, for example, containing the key words “kill yourself at school” amounted to 12,134 [11].
It is safe to say that there is a growing need for inpatient care for this category of patients in Moscow. To solve this problem, a Crisis Clinic was created at the Sukhareva Center in 2019 by order of the Moscow Department of Health [12].
The Crisis Clinic or Department of Critical Crisis Conditions, which is an integral part of the Sukhareva Center, specializes in helping children and adolescents aged 11 to 17 that suffer from autoagressive, including reactive or endoreactive, suicidal behavior.
The main principles upon which assistance at the Crisis Clinic is built are multi-disciplinarity (collective work amongst psychiatrists, psychologists, teachers, pediatricians, and other specialists), patient-centeredness (an individual approach to each case), staging of help with continuity of each stage, orientation towards the teenager’s family, and trust between patients and specialists.
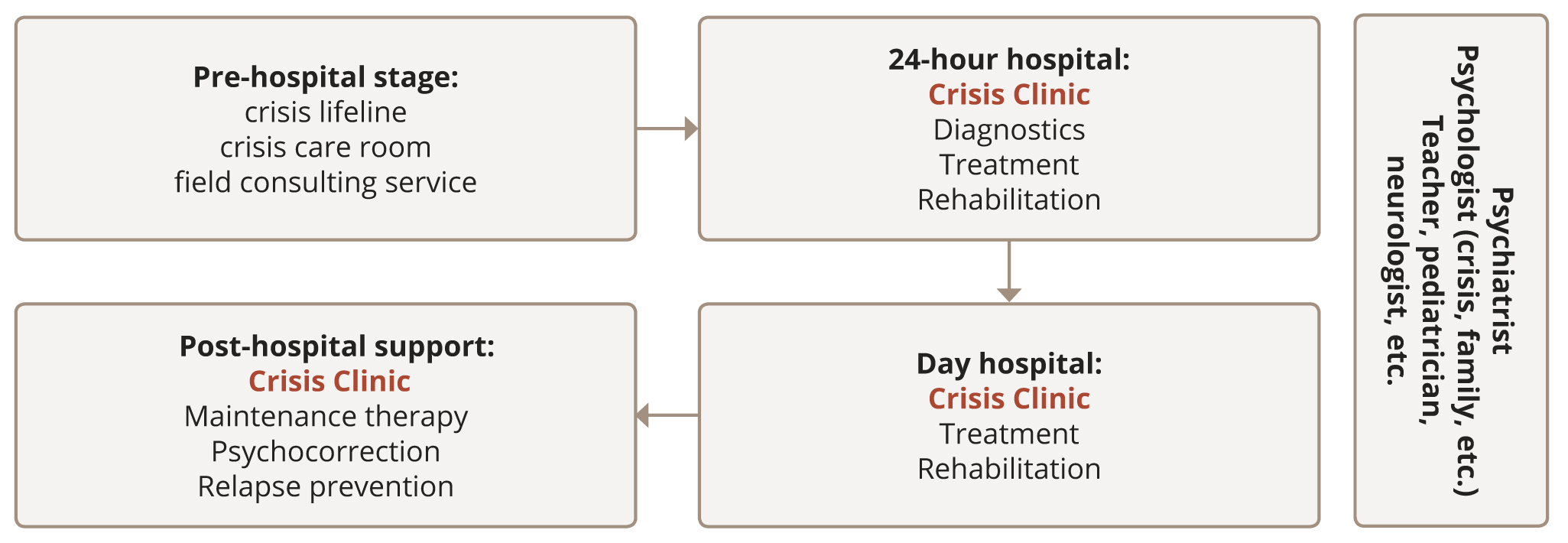
The Crisis Clinic is located in a large, one-story historical building (Medvednikovsky No. 14), surrounded by landscaped courtyards and promenade areas. The Crisis Clinic rooms are separate specialized structures — hospital part (including isolated rooms), day hospital, and post-hospital support office. This topology was dictated by the need to provide both a staged approach to crisis care and compliance with sanitary and epidemiological requirements. At the same time, maintaining the structural unity of the Crisis Clinic allows for the necessary continuity in the care to crisis patients by psychiatrists, psychologists, and specialists in family work, as well as educators, which promotes a higher quality of adaptation of patients during the transition to the next stage of treatment. The doctor and psychologist “receive” the adolescent and his family in the boxed area of the department (10 beds), “guide” them through the 24-hour hospital (30 beds), “pick them up” in the day hospital of the department (60 beds for patients), and support them after discharge in the office of post-hospital support (Figure 2).
Figure 2. The structure of the Crisis Clinic at the Sukhareva Center.
The Crisis Care Cabinet operates on the platform of the Sukhareva Center Clinical Diagnostic Department and provides emergency consultative medical and psychological assistance to children, adolescents, and their families in crisis. In addition to medical care and immediate decisions on necessary medical interventions, the office provides psychological help to the families of children in crisis, as well as family and individual counseling. Patients can show up at the office without first filling out an application form. Families with children and adolescents in crisis can receive counseling in the office without an appointment, on the day they present themselves. A therapist and a psychologist are both available at the office. During the first consultation, the level of crisis and severity of the patient’s condition are determined. If the child’s current condition threatens their life and health, and medical care must be provided immediately, emergency hospitalization is offered. If there is no need for emergency hospitalization, but there are indications for inpatient medical care, the patient and family are offered planned hospitalization at the Sukhareva Center, the specifics of the child’s condition, the reasons for which inpatient treatment is recommended, and the goals and objectives of hospitalization are explained.
At the first stage of hospitalization, patients are admitted to the adjacent unit that includes 8 isolated rooms with a total of 12 to 15 beds, intended for emergency hospitalization of patients in an acute crisis situation, including those referred by psychiatrists of the State Budgetary Institution of the city of Moscow “Station of Emergency Medical Care named after A.S. Puchkov” of the Moscow Health Department, district psychiatrists, and specialists from the consultative and diagnostic department of the Center. Isolation measures are taken until the results of the research are in hand, after which the child is transferred to the main section of the department. As soon as an adolescent is admitted to the department, they are examined by a team of specialists, including the head of the department, a child psychiatrist, and medical psychologists (a pathopsychologist, an individual psychologist, and a family psychologist). The priorities at this stage are solving diagnostic questions, determining the initial targets of individual and family psychological corrective work, and prescribing emergency psychopharmacotherapy, if needed.
As the appropriate examinations are conducted (on average, within 5–7 days), patients are transferred to the general hospital wards, the arrangement for which (up to 8 people per ward) is done taking into account clinical, as well as gender and age (including the grade of schooling), specifics. The organization of the wards is carried out with an emphasis on increasing the comfort of the patient’s stay and creating a favorable psychological (psychocorrectional) climate in the Department (including engendering an atmosphere of mutual help and support among patients and staff, the ability to store personal, items and toys that have a special meaning, clothing, the presence of “active” areas and lounging areas, regular meetings, and phone calls with parents, etc.). Additionally, the Department has specialized rooms for school and rehabilitation sessions, individual, group, and family psychological intervention.
The next stage in creating conditions for crisis resolution is the continuation of treatment in the environment of the Clinic’s day hospital. Children and adolescents report to the Crisis Clinic daily for the beginning of classes and procedures, while they may spend a significant portion of the day, as well as weekends, at home. Such a significant relaxation of routine requirements is possible if the patient and their relatives have been convinced to seek help and treatment and abandon the idea of suicide in the presence of good family support. At this stage, the entire scope of therapeutic and correctional measures begun in the 24-hour inpatient hospital is preserved, including school and rehabilitation classes, various psychological interventions, and the work of a family psychologist.
After a stabilization of the mental condition, elimination of the most pronounced psychopathological manifestations, and discharge, further observation of children and adolescents under crisis is performed on an outpatient basis in the psychiatric inpatient post-hospital support office. In such cases, the patients are treated by physicians and psychologists at the clinic, which ensures the necessary continuity and uninterrupted use of medication and therapy. The post-hospital support system is located in a separate wing of the Crisis Clinic and has a separate entrance, lobby, and sanitary block.
Between October 1, 2019, and September 30, 2022, crisis-room specialists conducted 8,481 consultations, with a total of 3,711 patients contacting the room during this period. Among them, 654 (17.6% of those contacted) were referred for emergency hospitalization with consultation in the office, and 1,542 (41.6%) were referred for planned hospitalization in the Center. The remaining patients received outpatient care in the office. The age of those who reached out for help ranged from 6 to 17 years, most often parents with adolescents applied to the office, and the most numerous contingent was adolescents aged 14–17 years. Girls were treated twice as often as boys. Patients were most often diagnosed with disorders from the groups F90–F98 “Emotional disorders, conduct disorders that usually begin in childhood and adolescence” (32.73%), F30–F39 “Mood disorders” (25.22%), and F40–F48 “Neurotic, stress-related and somatoform disorders” (18.36%).
From October 2019 to September 2022, 2,465 children (13.9% of all admissions) were admitted to the crisis unit. Most patients (76.4%) were admitted as emergency cases upon referral from the psychiatrist on duty at the “Station of Emergency Medical Care named after A.S. Puchkov” of the Moscow Health Department (44.8%) or upon direct admission to a psychiatrist at the Sukhareva Center (31.6%). At the same time, 72.6% of the children were hospitalized initially, 13.3% were repeatedly hospitalized, and 14.1% were repeatedly hospitalized within a year after the previous discharge.
The vast majority of children and adolescents (over 94.5%) admitted to the Crisis Clinic were living in their families, with 88 children (4.8%) being in foster care and only 9 patients (0.4% of all hospitalized) being institutionalized. School-age children were predominant among those admitted to the Crisis Clinic (more than 86.8%), with another 8.7% attending colleges and universities, with only 4.1% of the patients not enrolled in educational institutions.
The majority of children and adolescents admitted to the Crisis Clinic displayed some suicidal manifestations (62.07%). Among them, 14.93% were admitted after a suicide attempt, while the rest had suicidal thoughts and intentions.
Among the methods of realization of a suicide attempt in the general group of patients, vein dissection, poisoning, falling from a height, stabbing, strangulation, and hanging were predominent (Table 1).
Table 1. Methods used in suicide attemps among children and adolescents admitted to the Crisis Clinic between October 2019 and September 2022
|
Method |
Total group, % (n=2.465) |
|
Vein dissection |
50.5 |
|
Poisoning |
28.0 |
|
Falling from a height |
15.6 |
|
Stab wounds |
2.0 |
|
Asphyxiation, hanging |
2.4 |
|
Transport related methods |
1.0 |
|
Others |
0.5 |
|
Total |
100.0 |
The overwhelming majority of patients, along with suicidal behavior, experienced episodes of non-suicidal self-harm behavior (87%). The motive behind such behavior had to do with a desire to calm down, “to let off steam”, “to relieve tension”, etc. Self-injurious behavior was superficial, did not threaten the patient’s life, and was not conditioned by the intention to end one’s life.
For example, an adolescent 16–year-old girl had been making surface cuts on her forearms with a pencil sharpener blade over the past 2–3 years, usually after an argument with her parents or peers. She did not seek to kill herself, she was trying to “calm down” in this way, she took precautionary measures, including treating the cuts with antiseptic. At the same time, she did not deny having thoughts about not wanting to live, but she did not act on them.
More than 81.22% of the children and adolescents who sought help at the Crisis Clinic were young females. The average age of those admitted for treatment was 14.7 years and that of the boys was 15.0 years.
The diagnostic categories of all children and adolescents hospitalized between October 2019 and September 2022 were determined using ICD-10 criteria (Table 2). Depressive syndromes of various nosological affiliations dominated the clinical picture in the vast majority of children. The most frequently diagnosed were depressive episodes (39.8% F32) and disorders of emotions and behavior, with onset in childhood and adolescence (25.8% F92, F98). Schizophrenic spectrum disorders (15.1%); predominantly schizotypal disorder F21; and, even more rarely, stress-related neurotic disorders (10.9% F40–48) were observed less frequently. A small number of patients had eating disorders (F50 — 6.1%), organic brain damage (F06–07 — 1.6%), and mental retardation (F70 — 0.7%). The relatively small share of patients with neurotic and stress-related disorders can be explained by the fact that in many cases their manifestations at admission were considered to be symptoms of affective disorders, which are associated with age-specific features of the course of psychogenesis in children and adolescents in the form of an atypical and incomplete clinical picture and dynamics.
Table 2. ICD-10 diagnostic categories of patients admitted to the Crisis Clinic in 2019–2022
|
Diagnosis |
Total group, % (n=2.465) |
|
F31–F38 |
39.8 |
|
F92, F98 |
25.8 |
|
F20, F21 |
15.1 |
|
F40–F48 |
10.9 |
|
F06–F07 |
1.6 |
|
F50 |
6.1 |
|
F70 |
0.7 |
|
Total |
100 |
The central role in the care provided at the clinic is played by psychotherapeutic methods of treatment and rehabilitation: sessions with a family psychologist, individual and group work with a crisis psychologist, art therapy, clinical career guidance, sand therapy, dance and movement therapy, theater workshop, biofeedback, creative workshops, a cooking studio, and many more activities for the patient and their family. Corrective work is built around a family-oriented approach and consists of individual and group psychological corrective sessions, work with family psychologists, psychopharmacotherapy, physiotherapy, and medical and pedagogical remediation with the staff of the clinic.
Work with a family psychologist begins, as a rule, during the first week of hospitalization; parents and the teenager are invited to a meeting with the family psychologist; often, other family members are also invited. The subsequent format of intervention and frequency of meetings for each family is determined together with the attending physician and psychologists; the most standard frequency is 1–2 times a week. As a rule, during family therapy, parents and the teenager and sometimes only parents are assigned homework: the tasks can be very different, from the organization of board games to the creation of a family genogram — and performance of a task between meetings, along with the use of other original aids, is an important moment in the process of rehabilitation for the child.
No less important are individual and group psychological remediation sessions, which begin from the first days of the patient’s stay at the Crisis Clinic. Specialists at the Crisis Clinic have developed three original programs of psychological correction: intensive, basic, and supportive, and the choice of a particular program is made based on the opinions of the members of the multi-disciplinary team of specialists. Psychological care is focused on increasing psychological differentiation, which can manifest itself in an increase of emotional intelligence and the degree of self-control (development of adaptive coping strategies); in a qualitative transformation of self-awareness related to the separation and individualization of the personality, search for oneself; in improving the quality of cognitive and personal abilities related to the understanding and relevant evaluation of one’s capabilities, resources, and how they correlate with the desired qualities. The most successfully applied models, on which psychological help to children and teenagers is based, are the following: therapy based on mentalization (within the framework of the psychodynamic approach); functional behavior analysis, and training in functional communication (within the framework of the cognitive-behavioral approach); and communicative training directed at improving the quality of interpersonal interaction (for group work). Group psychological remediation sessions are presented in the following basic directions and variants: group skills (DBT, communicative training); “Me and Family”; body image and eating behavior; and stress management. To increase the effectiveness of psychologically corrective interventions with children and teenagers, the specialists at the Clinic developed original manuals (including workbooks for psychological sessions, individual and anti-crisis plans, etc.) and methods.
In addition, adolescents attend various therapeutic and remedial activities supervised by the Center’s rehabilitation units: cooking studios, classes in the theater studio, creative studio, photo club, DJ and guitar workshops, yoga, therapeutic physical training, painting, mime therapy, and more. Educational outreach projects of communication between patients and art historians in the form of lectures, master classes, and discussions take place regularly. One of the important areas of scientific and practical work at the Crisis Clinic and Sukhareva Center is the reduction of stigmatization of mental illness. In this area, discussion clubs, mental health festivals, lectures, and master classes are held with adolescents and parents.
Most patients at the Crisis Clinic receive psychopharmacotherapy with medications from various nomenclature groups, including neuroleptics, antidepressants, tranquilizers, and mood stabilizers. All medication is prescribed on an individual basis, at minimum or average age dosages, and with consideration of possible somatoneurologic side effects and age restrictions. Therapy with neuroleptics of mainly anxiolytic action (Alimemazine, Thioridazine, Chlorprotixen, etc.) and tranquilizers (Hydroxyzine, Tofizopam, Fabomotizole, etc.) are administered in the presence of acute or moderately acute neurological side effects and are used for acute and subacute anxiety disorders, while broader spectrum neuroleptics (Aripiprazole, Quetiapine, Clozapine, Paliperidone, Perphenazine, Risperidone, Sulpiride, etc.) are prescribed for endogenous and endoreactive depression in bipolar disorder. Antidepressants (Amitriptyline, Clomipramine, Sertraline, Pirlindol, Fluvoxamine, etc.) are also used to relieve depressive manifestations. Nomothetic drugs (Lamotrigine, Carbamazepine, salts of valproic acid, etc.) are used as a component of complex pharmacotherapy, in combination with neuroleptics and antidepressants. To suppress the development of side effects from the use of psychopharmacotherapy and any exacerbation of chronic somatic pathology, all patients are regularly examined by a pediatrician and, if necessary, by a neurologist, cardiologist, ophthalmologist, dentist, or gynecologist.
When we analyze the work of the Crisis Clinic, preliminary conclusions can be drawn about the effectiveness of the multidisciplinary approach, with a focus on family forms of assistance in the treatment of children and adolescents who display suicidal manifestations. Consequently, the analysis of the number of repeated hospitalizations compared to the involvement of family therapy suggests a decrease in the number of repeated hospitalizations, a more stable remission pattern, more significant compliance with therapy, and a decrease in the stigmatization of mental health services, which facilitates the further “management” of such patients.
The four years that have passed since the Crisis Clinic opened have shown how relevant it is, the effectiveness of its founding principles, and the need to involve the child’s family in all stages of their treatment and rehabilitation.