Consortium Psychiatricum
2021. Vol. 2, no. 3, 53–62
doi:10.17816/CP86
ISSN: 2712-7672 / 2713-2919 (online)
Community-Based Mental Health Services in Mexico
Abstract
AIM: This article describes the general characteristics of community-based mental healthcare in Mexico.
METHODS: Data from national surveys, special studies and statistics from the national information system during the period 2001–2017 are used. Available information on health systems, new regulations and the innovations implemented are reviewed, as well as research on psychosocial interventions conducted within the country.
RESULTS: Data show a fragmented health system with services for workers and those without social security or private care. This is a treatment system essentially based on tertiary healthcare and not integrated into the general health system, with a significant treatment gap and delay in relation to the first treatment. At the same time, a slow but steady increase in the level of care provided at primary healthcare level and in specialized community services has been observed. This trend has been accompanied by an increase in the number of medical doctors, psychologists and, to a lesser extent, psychiatrists, incorporated into the primary healthcare services. At the same time, no new psychiatric hospitals have been built; there has been a proportional reduction in psychiatric beds but no increase in mental health services or beds allocated to first contact hospitals. Research initiatives have analysed the barriers to reform, and efficient interventions have been developed and tested for the community and for primary healthcare; special interventions are available for the most vulnerable but no formal efforts have been to facilitate their implementation.
CONCLUSIONS: Evidence is available regarding the implementation of the transition from reliance on tertiary healthcare to reinforced primary care. At the same time, parity, financial protection, quality and continuity of care remain major challenges.
General Information
Keywords: mental disorders, treatment, community services, primary care, psychosocial interventions
Journal rubric: Special Articles
Article type: scientific article
DOI: https://doi.org/10.17816/CP86
Received: 05.07.2021
Accepted:
For citation: Cordero Oropeza M., Berenzon Sh., Robles R., Real T., Medina Mora M.E. Community-Based Mental Health Services in Mexico. Consortium Psychiatricum, 2021. Vol. 2, no. 3, pp. 53–62. DOI: 10.17816/CP86.
Full text
INTRODUCTION
The inclusion of mental health in the UN Sustainable Development Goals and the universal health coverage commitment adopted by countries, re-opened the debate on best practices in terms of closing the treatment gap between needs and the demand covered. This challenge posed in Alma Ata in 1978, namely, universal health coverage through primary care,1 has not been met around the globe2 and Mexico is no exception. The prevailing treatment paradigm, based on tertiary healthcare has failed and there is a large treatment gap in relation to both primary and specialized care (for example, only 19% of people with a mental condition and 49% of people with a substance use dependency have access to any care).3,4 This situation is compounded by the fact that those who are most at risk from mental health problems are usually those with the least access to services (i.e., families living in poverty, children exposed to abuse or neglect, minority groups or elderly people). Accordingly, a significant proportion of the population is excluded from mental healthcare.5,6
GENERAL HEALTHCARE SYSTEM IN MEXICO
The Mexican healthcare system comprises two sectors: public and private. Public services include social security institutions, which provide services for workers in the formal sector of the economy (IMSS) and the government (ISSSTE, PEMEX and others), and institutions that deliver services to those without social security. The private sector provides services for those with the capacity to pay.
Social security institutions are financed by government, employer and employee contributions, covering both employees and their families; students from public institutions, from 7th grade to postgraduate level receive free health services from these institutions.7 Services for the general population, not affiliated to any labour insurance, including freelance workers, those working for the informal economy, the unemployed, etc.), were funded by federal and state governments through the Popular Insurance Scheme, established in 2003. This scheme provided services for 40% of the population without medical insurance;8 a small contribution was paid by users when receiving care (recovery fees depending upon the income level).7 This system was substituted in 2019 by a new Institute of Health for Wellbeing (INSABI), which is still in the development stage. The private sector is financed through payments made by users when they receive care and through private health insurance premiums.7
The last available national health survey9 reported that 61% of outpatient consultations were provided by the public sector and 38.9% by the private sector, whereas only 17% of users of inpatient hospital services benefitted from services at private hospitals.
A recent report on Public Health and Primary Care,10 shows that despite significant reforms, key challenges remain. The National Health Survey9 showed that 21% of the population had no insurance, while a subsequent survey revealed that 87% of the population from the lowest socioeconomic level lacked access to health services. It has also been estimated that 49% of health expenditure is private and that over 90% corresponds to out-of-pocket expenses, mainly for outpatient care and medicines.
THE HISTORY OF MENTAL HEALTH SERVICES
Mental health services have been provided at psychiatric institutions since 1566. For many years, treatment was based in psychiatric hospitals, with little investment in rehabilitation or community care.11 Mexico was one of the few countries to participate in the World Mental Health Survey,12 which demonstrated that it is one of the countries with more people seen at the tertiary care level than at the primary care level.13 Thus, latency in receiving care is high: 14 years for depression as opposed to one year in Spain.14,15
Primary care services for mental health also have a long history. The Mexican Institute of Social Security (IMSS) recognized the need for family doctors in 1954, however, it was not until 1971 that the specialization of family medicine was created, with a focus on primary care (86% of its services). Psycho-affective disorders are among the 10 leading reasons for consultation.16
For persons not affiliated to the IMSS, primary care services were formalized in 1959 after the Ministry of Health established the General Directorate of Neurology, Mental Health and Rehabilitation. This, in turn, created the Mental Hygiene Services, incorporated into primary care centres in Mexico City, with preventive actions and first contact care, and a referral system to specialized services. The staff was multidisciplinary with a psychiatrist, psychologist, and social worker. This initiative was not widespread and by 1964 only 16 such services had been established, 10 in Mexico City and six in various states. In the 1980s and 1990s, the federal authorities overhauled the health sector, reducing the budget and the range of services, including mental healthcare.17,18
The Ramón de la Fuente National Institute of Psychiatry, a national health institute with research, education and clinical services was inaugurated in 1979. Research into the epidemiology of mental disorders, neurosciences, as well as clinical and psychosocial aspects led to culturally adapted interventions. Emphasis was placed on the more vulnerable and new models were tested in communities, primary care and specialized services.19,20
Mental health was included in the Popular Insurance Scheme via payment to each state, depending on the local quota per affiliated family. In 2007, prevention (e.g., early detection and brief advice for addictions), screening and treatment (pharmacological and psychotherapeutic) for various mental health disorders were included. The number of disorders covered increased over time and by 2018, the scheme covered autism, depression and other mood disorders, as well as psychosis.21 Unfortunately, this was not fully implemented as a primary care referral to tertiary level was required, among other reasons, with limited hospitalization days and a re-referral to primary care for the continuity of care; care for severe depression was only provided in general hospitals, but the institutions were not ready to identify or treat those with mental disorders; as a result the provision for mental disorders was poor. The health budget in 2017 was
1.00 per capita, while in high-income countries it was, on average, $58.73.22 When the Popular Insurance Scheme was established, public expenditure on mental health increased from 0.3% to 0.7%, then declined continually to a level of 0.3% by 2017. Although the new government has announced the implementation of a new program to replace the former Popular Insurance Scheme and has committed to universal coverage, there has been a significant reduction in the health budget since 2019. However, patients with mental disorders, who receive treatment in public institutions, are beginning to have access to free medication (https://ciep.mx/presupuesto-para-salud-mental-relevancia-ante-la-covid19/).
The trend is shifting care delivery from psychiatric institutions to community-based services, and there has been a growing involvement of primary healthcare.23 In 2012, 42 specialized medical units for ambulatory care were opened in 20 states. In 2018, before the COVID-19 pandemic, 51 units were operating in 22 of the 32 Mexican states.24 Three hundred and ten centres were also opened for the prevention and treatment of substance use disorders, yet despite the common comorbidity,25 mental healthcare was not included in their mandate initially;26 however, in 2019 a reform mandated treatment of mental and substance use disorders in both systems. A third organization, Juvenile Treatment Centres (CIJ) for substance use disorders, with 120 community centres, also included mental health treatment. Today, the three organizations are united within a network that has amplified health coverage significantly.
Unfortunately, there is still no formal referral system for mental disorders among the different levels of care. Individuals seen at primary care level are often referred to the tertiary level without treatment. This is primarily because primary level medical consultations are usually brief and focus on treating somatic symptoms, making the detection and treatment of chronic disorders more difficult. This is compounded by the lack of collaboration between primary care staff (mainly general and family doctors, nurses, psychologists and social workers) and mental health specialists, and the lack of trained human resources to deliver mental healthcare, including psychiatrists.5,27
The country has also made significant progress in formulating laws, policies and programs to improve community mental healthcare, which comply with international human rights guidelines and are periodically reviewed. However, these have only been partially implemented. In this respect, the seventh chapter of the Mexican General Health Law stipulates the characteristics of mental healthcare. Likewise, certain states, including Mexico City, have a specific mental health law, stating that the prevention and care of mental illness is a priority for the government. In recent years, various initiatives have been submitted to the Senate and the Chamber of Deputies to establish a National Mental Health Law, aimed at promoting community services, strengthening primary healthcare, outpatient care and coordination with hospitalization systems.
GENERAL CHARACTERISTICS OF THE MENTAL HEALTH SYSTEM
Mexico allocates 2.2% of the total health budget to mental health services, eight times lower than the proportion of the global burden of disease, estimated for mental health disorders (16% of the total days lost for premature mortality and days lived without health; conversely, 80% is spent in the tertiary care sector).5,23,28 To serve a population of 129.2 million inhabitants, there are 39 psychiatric hospitals in Mexico, 34 of which are funded by the Ministry of Health and five by the National Institute of Social Security. These psychiatric hospitals provide care for workers and families with mental disorders, with an organized referral system, yet characterized by significant treatment delays. Services for government workers provided by ISSSTE are delivered by the public sector and 89% of hospitals are located in major cities.
Psychiatric hospitals have extended outpatient services. Although patients can be referred by other hospitals or primary healthcare workers, they usually seek outpatient and inpatient care at psychiatric hospitals without a referral. Only 2% of the beds are in general hospitals. There are 1649 mental health community services, 467 of which were developed as part of the initiative to bring specialized outpatient services to the community, known as UNEMES, and 1169 primary care units within the mental health service.
In 2017, 3.3 million medical consultations were provided by the Ministry of Health for individuals without social security (1.2 million, nearly a third, were provided by the Popular Insurance Scheme) and for those with social security, as mental health services in this sector are limited. Of the total number of medical consultations by the Ministry of Health, 24.8% were provided in the outpatient services of psychiatric hospitals and 20.7% by other specialized hospitals, with a total of 45.5% being provided at tertiary care level. Approximately the same proportion (45.4%) was provided in outpatient mental health services (of which 28.4% were provided in general health centres with mental health services and 17% at outpatient mental health clinics), an important shift since 2010, when only 38.3% of medical consultations were provided by outpatient mental health services. In 2017, only 8% were provided in general hospitals with mental health services.
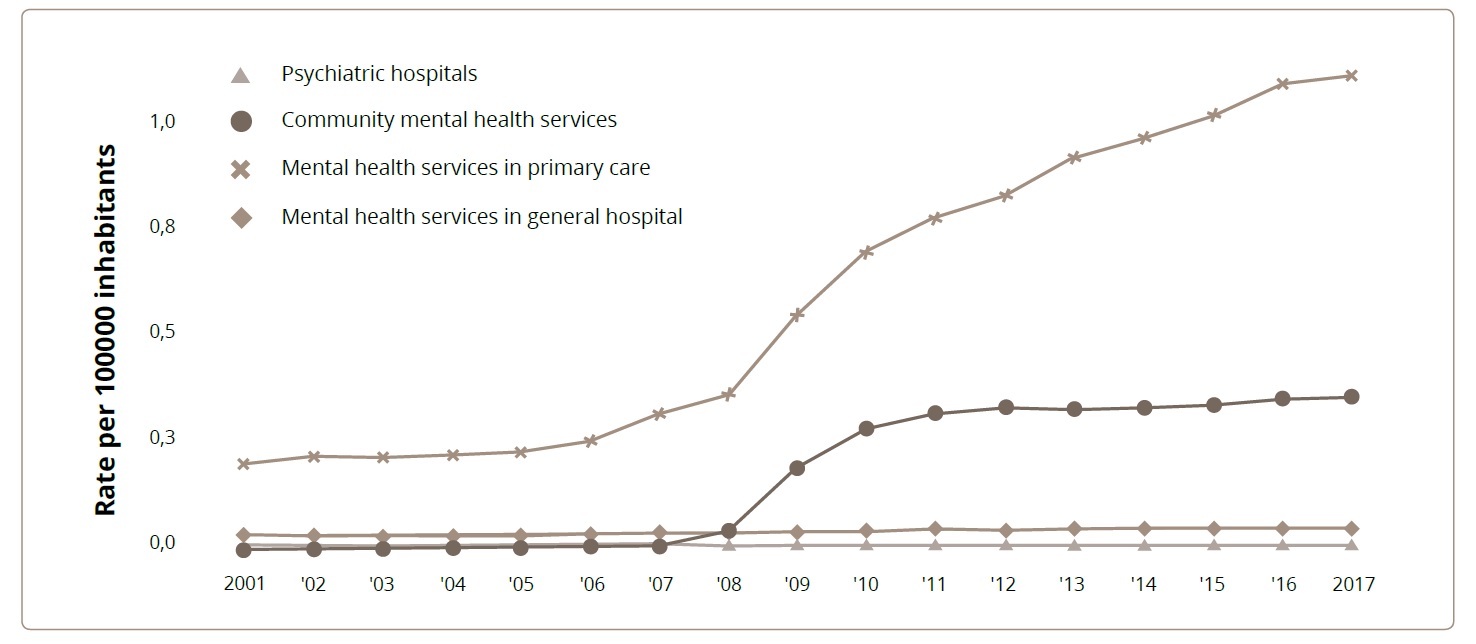
Trends in mental health services can be observed within the units run by the Ministry of Health. Data show a sustained increase in primary health units with mental health services (rising from 0.2 per 100,000 inhabitants in 2001, to 1.1 per 100,000 inhabitants in 2017). Since 2008, there has also been an increase in mental health community services (from 0.1 per 100,000 inhabitants in 2008 to 0.4 per 100,000 inhabitants in 2017) (Figure 1).
Figure 1. Trends in the availability of Mental Health Services
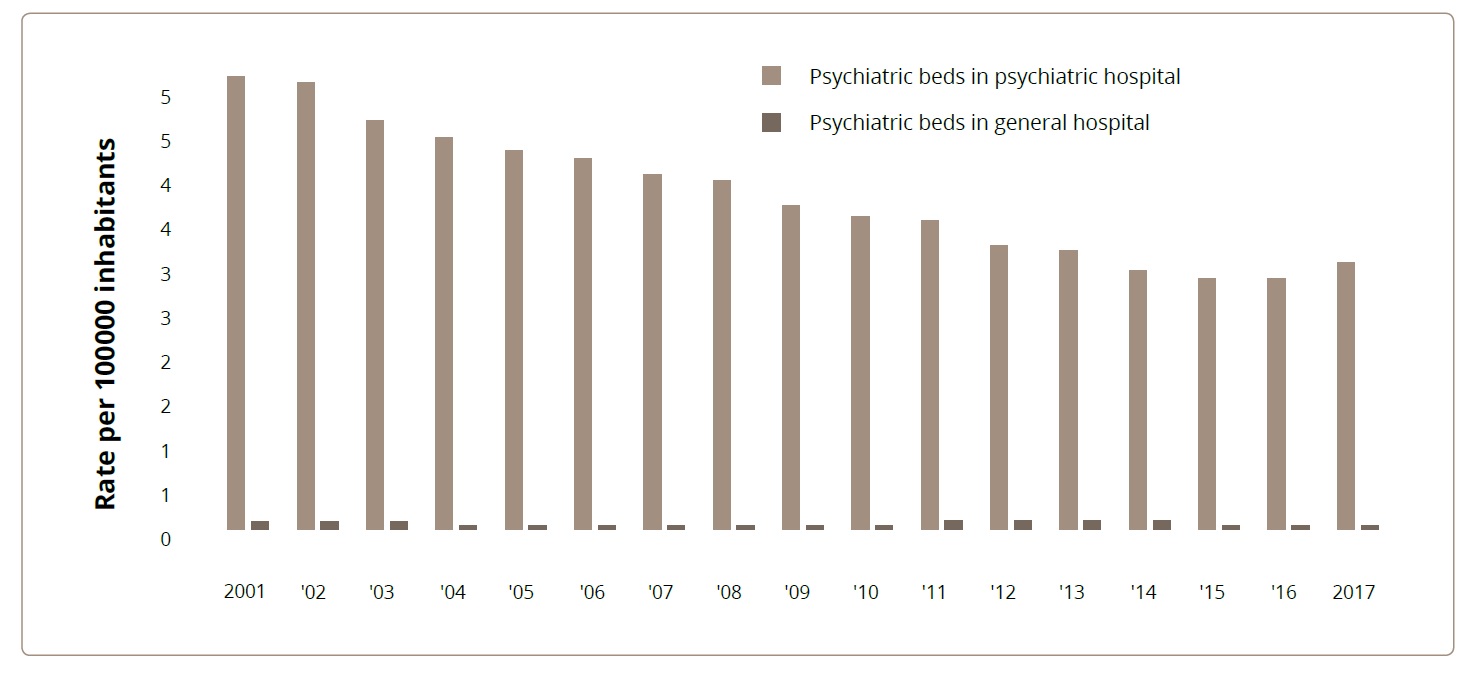
The number of psychiatric hospitals has remained stable (with 0.03 hospitals per 100,000 inhabitants). Although the number of beds in psychiatric hospitals decreased from 5.07 to 2.98 per 100,000 inhabitants, psychiatric beds in general hospitals did not increase (Figure 2).
Figure 2. Trends in the distribution of beds and psychiatric services
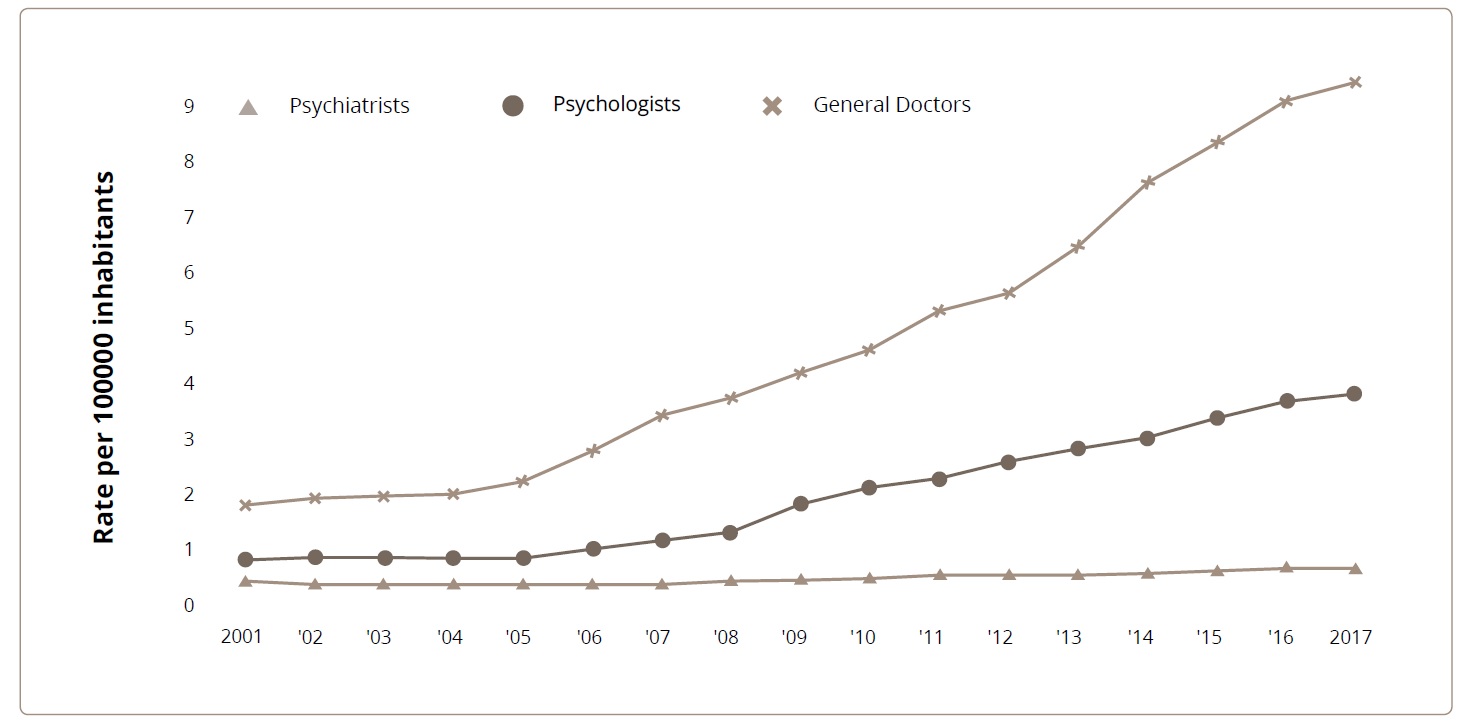
Coinciding with this trend in services, human resources have also increased. From 2001 to 2017, within the services coordinated by the Ministry of Health, the number of psychiatrists rose from 0.5 to 0.7 psychiatrists per 100,000 inhabitants; GPs working in mental health services increased fivefold (from 1.9 to 9.5), while the number of psychologists increased fourfold from 0.9 to 3.9 psychologists per 100,000 inhabitants (Figure 3).
Figure 3. Human Resources in Mental Health Services
From 2010 to 2017, outpatient mental health in primary care accounted for 38.5% of all outpatient consultations, reaching 45.4% in 2017 (primary care units within the mental health service rose from 22.5% to 28.4%, while community mental health units increased from 15.8% to 17.0%). Conversely, outpatient care at highly specialized hospitals decreased from 21.5% to 20.7%, while outpatient care at psychiatric hospitals fell from 29.3% to 24.8% during this period.
More than half of all hospital discharges (62%), due to mental and behavioral disorders were from psychiatric hospitals, 24% were from general hospitals, 9.1% were from specialized hospitals and 4.4% from rural hospitals.
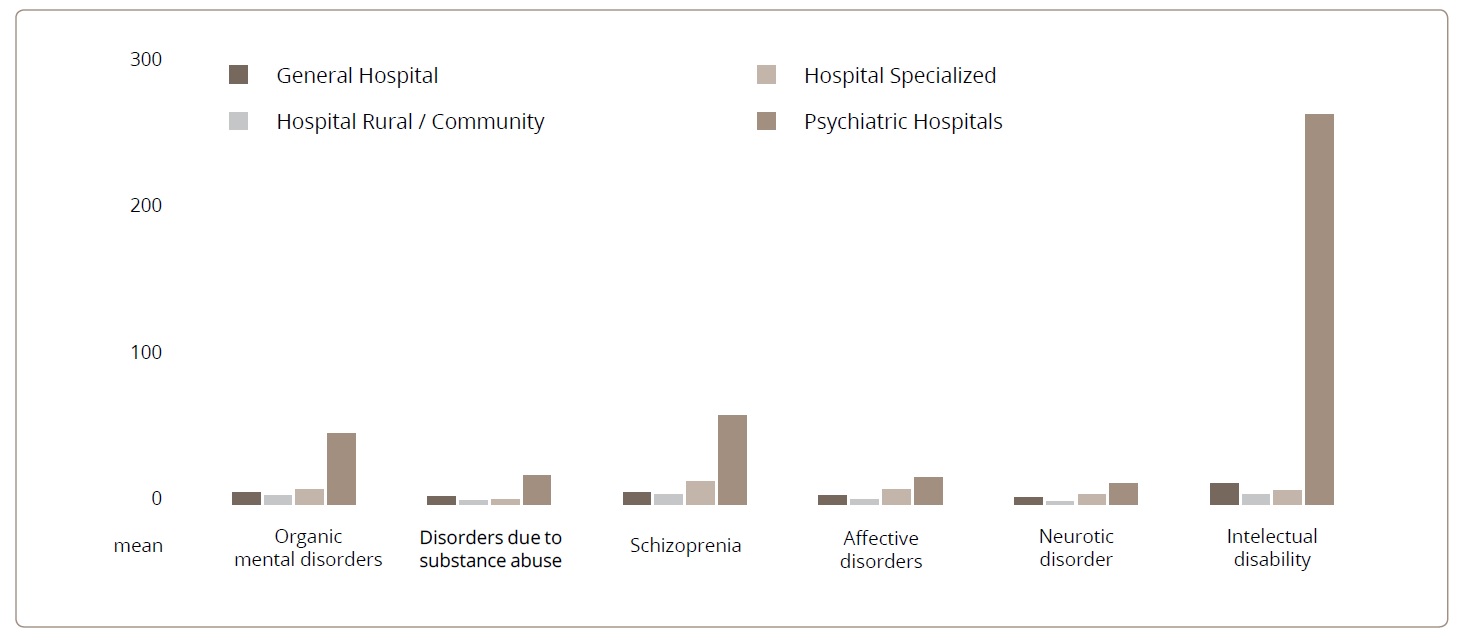
Inpatient care days varied according to the type of disorder and the characteristics of the care services. Psychiatric hospitals had the longest stays of all services for all disorders, except for personality disorders, the duration of which was the same in psychiatric hospitals and specialized hospitals. Intellectual disability involved the lengthiest stays (from 263 days in psychiatric hospitals to 6.6 days in hospitals located in rural communities) (Figure 4).
Figure 4. Average of inpatient days in hospital due to mental
GENERAL CHARACTERISTICS OF COMMUNITY-BASED MENTAL CARE IN MEXICO: INTERVENTIONS
The delivery of community-based mental care takes place in schools, workplaces and through the families of the most vulnerable. The treatment developed and tested by the National Institute of Psychiatry (INPRFM) includes programs for those with mental disorders and their families,31 on-line interventions for depressed females who have not sought help32 (assistance) to reduce substance use and depression symptoms,33 interventions for families with alcohol-related problems in indigenous populations,34 prevention of violence among young people35 survivors of violence, street children and youth, prison populations, sex workers, migrants, those living in unsafe communities, indigenous groups, as well as communities living in poverty.36
The principal, evidence-based psychological interventions that have proven to be effective in Mexico include cognitive-behavioral techniques (such as behavioral activation, relaxation training for anxiety and identification, and modification of automatic thoughts related to depression and anxiety), implemented in rural community health settings,37 as well as problem-solving therapy,38,39 stress reduction based on mindfulness training40 and stress management for mental health professionals.41
There have also been local efforts to complement pharmacological and psychological interventions, designed to address the contextual sources or social determinants of mental health problems (such as underemployment, inadequate housing, food insecurity, and violence) through the collaborative work of primary care providers (PCP) and promoters (trusted community members, who deliver health-related services).42
Initiatives to help general practitioners overcome the barriers of lack of time and expertise, as well as the evaluation and management of common mental disorders observed in the primary care setting (i.e., depression, anxiety and unexplained medical symptoms) have been implemented and evaluated in Mexico (including very brief screening tools, training packages on WHO-mhGAP guidelines and manualized psychological interventions).43,44
STRENGTHS, WEAKNESSES AND FUTURE DEVELOPMENTS
It is true that public policies exist to guide actions designed to care for the community and that significant progress has been made in the development of community-based care services. However, although some progress has been observed in terms of a greater participation in primary care, the treatment for mental disorders remains within specialized services (tertiary care), specifically psychiatric hospitals. These hospitals remain responsible for a large proportion of outpatient care and nearly all hospitalizations. The shift towards a paradigm of more community than hospital care has been hampered by the lack of an integrated policy and an insufficient, poorly optimized budget.
A clear example of these conditions is the low availability of psychotropic drugs in primary healthcare, forcing people to buy them out of pocket, which either has a major impact on a family’s finances and/or prompts the decision not to take the medication. Low priority is attributed to mental health because in many cases, it is still considered the exclusive domain of specialists in the mental health sector. Many patients with mild disorders, which are under control and can be treated in primary healthcare, are referred to psychiatric hospitals.
It is essential to allocate more financial resources and to distribute them more effectively to enhance community mental health. Likewise, care models with successful results should be promoted, taking into account the impact of social, cultural and environmental factors on mental illness.
One of the elements that has worked least well in Mexico is the participation of patients in the community. Self-management is rarely promoted, and actions taken by community members are not fully exploited, such as linking MH services with the population by recommending available social networks. It is necessary to promote actions to expand and coordinate the participation of community members and patients, encouraging them to take care of their mental health and helping them recognize when to seek services. The World Health Organization also recommends the participation of patients and family members in the planning and implementation of policies, and the monitoring and provision of services.
Likewise, to improve the delivery of community services in Mexico and to achieve a model, such as that proposed by the WHO, it is essential to strengthen communication and collaboration between the various platforms45 and to set up continuous monitoring systems. This link between the community and the health system will facilitate the identification of cases, care seeking and the timely referral to treatment.
One of the challenges is to achieve a paradigm shift whereby mental healthcare is not only the responsibility of psychiatrists and psychologists. The results of various investigations confirm that other health professionals (nurses, social workers) and even those from the same community could carry out mental health promotion activities, as well as the detection and care of certain mental disorders, with the appropriate training, supervision and continuous support from mental health specialists.
CONCLUSIONS
A small but steady increase in services and human resources (more GPs and psychologists) in primary healthcare and specialized community services was observed. This shift is an important step towards reducing the treatment gap.
The challenge for the population that does not have a severe psychosocial disability, is to assess the scope of these actions to reduce the treatment gap for mental disorders, and to ensure the quality and continuity of care. We are convinced that Mexico can build a mental healthcare model that will improve the quality of life of the population, by integrating mental healthcare across the lifespan into the health system, with coordinated actions in various sectors, including civil society organizations.
No additional psychiatric hospitals have been built and the number of beds at these institutions has declined. Unfortunately, there has not been an increase in the number of beds or mental health services in general hospitals. A significant proportion of persons with mental disorders are in jail.46 Those with a severe intellectual disability and to a lesser extent, schizophrenia and other psychoses, are abandoned in the isolation wards of long-stay psychiatric hospitals. This calls for an urgent program of deinstitutionalization to smaller units, with the necessary services to protect the human rights of this population, together with a new system to guarantee continuity of care, housing and labour facilities, so as to integrate those with psychosocial disabilities into the community.
References
- World Health Organization, United Nations Children's Fund. Primary health care: report of the International Conference on Primary Health care, Alma-Ata, USSR, 6-12 September 1978. World Health Organization; 1978.
- Patel V, Saxena S, Lund C, et al. The Lancet Commission on global mental health and sustainable development. Lancet. 2018;392(10157):1553-1598. doi: 10.1016/s0140-6736(18)31612-x
- Medina-Mora ME, Borges G, Lara Muñoz C, et al. Prevalencia de trastornos mentales y uso de servicios: Resultados de la encuesta nacional de epidemiología psiquiátrica en México. Salud Mental. 2003;26(4):1-16.
- Reséndiz Escobar E, Bustos Gamino MN, Mujica Salazar R, et al. National trends in alcohol consumption in Mexico: results of the National Survey on Drug, Alcohol and Tobacco Consumption 2016-2017. Salud mental. 2018;41(1):7-16. doi: 10.17711/sm.0185-3325.2018.003.
- Berenzon S, Saavedra N, Medina-Mora ME, et al. Evaluación del sistema de salud mental en México: ¿hacia dónde encaminar la atención? Rev Pan Salud Pública. 2013;33(4):252-58.
- Urbina M. Los determinantes sociales de la salud y la salud mental. In: Mora MEM, Sarti Gutierrez EJ, Quintanar TR, eds. La Depresión y Otros Trastornos Psiquiátricos. Documento de Postura. Academia Nacional de Medicina; 2015: 409.
- Gómez-Dantés O, Sesma S, Becerril VM, et al. Sistema de salud de México. Salud Públ Méx. 2011;53(2):S220-S232.
- Ávila-Burgos L, Serván-Mori E, Wirtz VJ, et al. Effect of Seguro Popular on health expenditure in Mexican households ten years after its implementation. Salud Públ Méx. 2013;55(2):S91-S9.
- Gutiérrez JP, Rivera-Dommarco J, Shamah-Levy T, et al. Encuesta Nacional de Salud y Nutrición 2012. Resultados Nacionales. Instituto Nacional de Salud Pública; 2012.
- Rivera J, Pérez R, Reyes H, et al. Salud Pública y atención primaria. Base del acceso efectivo a la salud de los mexicanos. Instituto Nacional de Salud Pública; 2018.
- Berenzon S, Lara MA, Robles R, Medina-Mora ME. Depresión: estado del conocimiento y la necesidad de políticas públicas y planes de acción en México. Salud Pública de México. 2013;55(1):74-80.
- Medina-Mora ME, Borges G, Benjet C, Lara C, Berglund P. Psychiatric disorders in Mexico: lifetime prevalence in a nationally representative sample. Br J Psychiatry. 2007;190:521-528. doi: 10.1192/bjp.bp.106.025841.
- Wang PS, Angermeyer M, Borges G, et al. Delay and failure in treatment seeking after first onset of mental disorders in the World Health Organization's World Mental Health Survey Initiative. World Psychiatry. 2007;6(3):177-185.
- Borges G, Wang PS, Medina-Mora ME, Lara C, Chiu WT. Delay of first treatment of mental and substance use disorders in Mexico. Am J Public Health. 2007;97(9):1638-1643. doi: 10.2105/AJPH.2006.090985.
- Alonso J, Liu Z, Evans-Lacko S, et al. Treatment gap for anxiety disorders is global: Results of the World Mental Health Surveys in 21 countries. Depress Anxiety. 2018;35(3):195-208. doi: 10.1002/da.22711.
- Dávila J, Garza MG. Medicina Familiar. Editorial Alfil; 2013.
- Benassini FO. La atención psiquiátrica en México hacia el siglo XXI. Salud Mental. 2001;24(6):62-73.
- Martínez G. Un sistema en busca de salud: Desarrollo, declive y renovación del sistema de salud mexicano. Fondo de Cultura Económica; 2013.
- De la Fuente R. Semblanza de la Salud Mental en México. Salud Públ Méx.1998;30(6):861-71.
- Medina-Mora ME, Berenzon S. Salud Mental y Adicciones. Agenda Ciudadana de Ciencia, Tecnología e Innovación. DGD, UNAM/AMC/CONACYT; 2013.
- Comisión Nacional de Protección Social en Salud. Causes 2019. Catálogo Universal de Servicios de Salud. Secretaría de Salud; 2019.
- Senyacen J. Gasto en Salud Mental. Salud y Finanzas Públicas. Centro de Investigación Económica y Presupuestaria, A. C. 2017. Accessed August 30, 2021. https://ciep.mx/gasto-en-salud-mental.
- Madrigal de León EA. Fortalecimiento de la salud mental en México: recomendaciones para una psiquiatría comunitaria. Salud Mental. 2016;39(4):235-237.
- Secretaría de Salud. Acciones y Programas del Secretariado Técnico del Consejo Nacional de Salud Mental. México. Accessed August 30, 2021. https://www.gob.mx/salud/documentos/acciones-y-programas-del-secretariado-tecnico-del-consejo-nacional-de-salud-mental.
- Marín-Navarrete R, Benjet C, Borges G, et al. Comorbilidad de los trastornos por consumo de sustancias con otros trastornos psiquiátricos en Centros Residenciales de Ayuda-Mutua para la Atención de las Adicciones. Salud Mental. 2014;36(6):471-479.
- Consejo Nacional Contra las Adicciones. Programa de Acción Específico. Prevención y Atención Integral de las Adicciones. Actualización 2011-2012. Consejo Nacional Contra las Adicciones; 2012.
- Berenzon-Gorn S, Saavedra-Solano N, Galvan-Reyes J. Contexts and challenges for mental healthcare at the first level. A socioecological approach. Contextos y desafíos para la atención de la salud mental en el primer nivel. Una aproximación socio ecológic. Salud Publica Mex. 2018;60(2):184-191. doi: 10.21149/8673.
- Organización Panamericana de la Salud. La carga de los trastornos mentales en la Región de las Américas, 2018. OPS; 2018.
- Consejo Nacional de Población. Proyecciones de la Población de México y de las Entidades Federativas, 2015-2050. Accessed August 30, 2021. https://datos.gob.mx/busca/dataset/proyecciones-de-la-poblacion-de-mexico-y-de-las-entidades-federativas-2016-2050.
- Secretaría de Salud. Subsistema de Prestación de Servicios. Accessed August 30, 2021. http://www.dgis.salud.gob.mx/contenidos/intercambio/Info_guia_SIS_CE_gobmx.html.
- Rascón Gasca ML, Hernández Durán V, Casanova Rodas L, et al. Guía Psicoeducativa para el Personal de Salud que brinda Atención a Familiares y Personas con Trastornos Mentales. Instituto Nacional de Psiquiatría Ramón de la Fuente Muñiz. Serie: Guías Clínicas para la Atención de Trastorno Mentales; 2010.
- Lara MA, Tiburcio M, Aguilar AA, Sánchez-Solís A. A four-year experience with a Web-based self-help intervention for depressive symptoms in Mexico. RevPanam Salud Pública 2014;35(5-6):399–406.
- Tiburcio M, Lara MA, Aguilar Abrego A, et al. Web-Based Intervention to Reduce Substance Abuse and Depressive Symptoms in Mexico: Development and Usability Test. JMIR Ment Health. 2016;3(3):e47. doi: 10.2196/mental.6001.
- Natera G, Medina P, Calleja F, et al. Efectos de una intervención a familiares de consumidores de alcohol en una región indígena en México. Salud Mental. 2011;34:195-201.
- Ramos L, Fuentes P, Flores K, Ruíz E. Evaluación de una intervención en línea para prevenir la violencia en población juvenil y adolescente. Resultados preliminares sobre su efectividad con profesionales de la salud. Salud Mental. 2014;37(3):195-204.
- Fuentes P. Intervenciones selectivas en salud mental. In: Medina-Mora ME, Sarti J, Quintanar TR, eds. La Depresión y Otros Trastornos Psiquiátricos. Documento de Postura. Academia Nacional de Medicina; 2015:409.
- Páez F, Robles R, Chávez J. Eficacia de una intervención psicológicaimpartida por un pasante de medicina para disminuir la sintomatologíadepresiva y ansiosa en mujeres rurales del estado de Jalisco. Trabajo deInvestigación presentado en el Encuentro Nacional de Investigadores. Secretaría de Salud; 2002.
- Vargas BE, Villamil V. La salud mental y la atención primaria en México. Experiencias de un modelo de atención colaborativa. Salud Mental. 2016;39(1):3-9. doi: 10.17711/SM.0185-3325.2015.062.
- Villamil V, Vargas BE, Caraveo J, et al. Glucose and cholesterol stabilization in patients with type 2 diabetes mellitus with depressive and anxiety symptoms by problem-solving therapy in primary care centers in Mexico City. Prim Healthcare Res Dev. 2018;19(1):33-41. doi: 10.1017/S1463423617000512.
- Bernal PR. Evaluación de un programa de reducción de estrés basado en la atención plena para mujeres con enfermedades crónicas, sintomatología ansiosa y/o depresiva en el primer nivel de atención. Dissertation. Universidad Nacional Autónoma de México; 2018. Accessed August 30, 2021. http://132.248.9.195/ptd2018/octubre/0781995/Index.html.
- Fuentes P, Barrera MI, Forteza C, et al. Evaluación de la efectividad de una intervención interactiva para el manejo del estrés en profesionales de la salud. Salud Mental. 2015;38(5):347-351.
- Stacciarini J-MR, Rosa A, Ortiz M, et al. Promotoras in Mental Health. Fam Community Health. 2012;35(2):92-102. doi: 10.1097/FCH.0b013e3182464f65.
- Goldberg DP, Reed GM, Robles R, et al. Screening for anxiety, depression, and anxious depression in primary care: A field study for ICD-11 PHC. J Affect Disord. 2017;213:199-206. doi: 10.1016/j.jad.2017.02.025 doi: 10.1016/j.jad.2017.02.025.
- Robles R, Lopez-Garcia P, Miret M, et al. WHO-mhGAP Training in Mexico: Increasing Knowledge and Readiness for the Identification and Management of Depression and Suicide Risk in Primary Care. Arch Med Res. 2019;50(8):558-566. doi: 10.1016/j.arcmed.2019.12.008.
- Shidhaye R, Lund C, Chisholm D. Closing the treatment gap for mental, neurological and substance use disorders by strengthening existing healthcare platforms: strategies for delivery and integration of evidence-based interventions. Int J Ment Health Syst. 2015;9:40. doi: 10.1186/s13033-015-0031-9.
- Almanzar S, Katz C, Harry B. Treatment of mentally ill offenders in nine developing Latin American Countries. J Am Acad Psychiatry Law 2015;43(3):340-349.
Information About the Authors
Metrics
Views
Total: 27
Previous month: 3
Current month: 2
Downloads
Total: 7
Previous month: 0
Current month: 0